I always assumed my experience as a veterinarian would serve me at some point when I needed to navigate the human healthcare system. The similarities between veterinary training and medical training, after all, lend themselves to a good number of similarities: how to read scientific articles critically. How to read an MRI. When to call the office and say, this prescription doesn’t seem quite right, is this what you wanted?
The similarities are all well and good, but I never understood, in the marrow of my bones, until recently that what would serve me best was our differences.
We MDs and DVMs are both given an ethical mandate to ‘do no harm’, which we as communities hold dear. Our duties to our patients are guided by this overarching principle; we look to it for direction in complicated cases, fall back on it when we feel conflicted about a request, and hold it like a flashlight when we shine a light into the cave of an uncertain future, looking for direction.
But oh, do those lights shine in very different spectrums.
Recently, a man in Russia volunteered to become the subject of the very first head transplant, an idea that leaves most of the world recoiling in horror. “There are some things worse than death,” said many of the neurosurgeons commenting on the piece.
As a veterinarian, I agree. We veterinarians occupy a strange place in the medical field in that most of us view it as not only an option but often a moral imperative to ease the pain of a traumatic death process through pharmacologic means. We are precise in our process, with the goal of minimizing stress and pain. We view it not as causing death, but as easing an uncurable pain. In this, we view our fulfillment to do no harm.
But in the human medical field, the prevailing attitude is by and large that hastening death is, indeed, harm, and anything we do to prolong a life is conversely fulfilling their requirement to do no harm, no matter what it does to a person or family in the process.
Even if it is multiple craniotomies.
Months of chemotherapy.
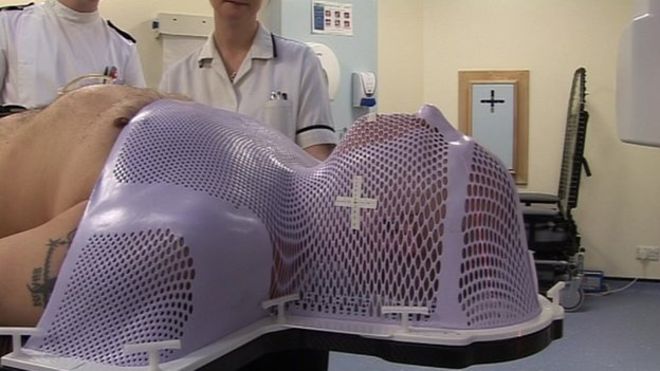
Daily radiation therapy with a bevy of ill effects. And you have to get screwed down to the table wearing one of these while they shoot brain shrivelling radiation beams at your head:
Not to cure a disease, but to make a patient breathe one more day, for better or for worse. It is the second most common utterance to me in my hospice work: we do better with our pets than we do our people when it comes to end-of-life decisions, and truly, friends, we really do.
I was recently-by invitation- listening to a doctor outline just such a series of events and possibilities to a patient who didn’t want to partake in them, who has been looking- without success- for someone to say, it’s ok to say no to months of hospital visits and yes to fewer days filled with this:
Plenty of people do want everything we have to throw at disease, and more power to them all. Thank God for modern medicine. But when did it become not only an unthinkable mistake, but an outright affront to the medical community to say, “thanks but no thanks”?
Searching for information on hospice and palliative care has been as challenging as getting bootleg rum during prohibition, furtive conversations in hallways and whispered hints at such necessary things as family support and respite care, secondary concerns far down the to-do list after scheduling yet another CT. I never knew how much of an afterthought the emotional wellbeing of the patient truly is in many medical decision making processes.
“So what if they don’t want to do this?” I asked.
“Well, this is the standard of care,” the resident responded.
“And if they choose not to do this?” I asked again.
“Why wouldn’t you?” he said, dumbfounded. He never did give me an answer.
Do no harm.







Once again…. Amen! Recently a woman had premature labor and gave birth to 22 week twins at the hospital where i work. She and her husband did not want resuscitation. The MDs said, but look they are breathing! So they shoved tubes down their throats and IV’s in extremities and called it a success. I don’t think the parents feel the same. Tragic indeed.
<3
This! SO much this. Thank you for all that you do Dr. V!
Thank you, thank you, thank you!!! I love your blog, you always seem to hit it right on the head. The human medical community just doesn’t get it. There are folks that don’t want to prolong there life if they can’t at least do some of the things they love to do and have no or little pain. We are more caring to our pets than we are to our self.
Perfectly said. I recently lost my 13+yo Doberman, Sabrina, to what we think was osteosarcoma in her front leg. As a person who used to work in the veterinary field, my vet is always honest and up front with me – no candy coating anything, no false hopes, no beating around the bush. My choices for Sabrina’s treatment were: 1. Do a biopsy, then go see an oncologist. 2. Amputate 3. Amputate, then do chemo and radiation or 4. Treat the pain.
I chose to treat the pain. Sabrina had terrible arthritis in her hind legs. How would she be able to walk with one good front leg?! And at her age, the adjustment of losing a leg would have been so hard on her. We had her for 16 days after her diagnosis. She couldn’t get around on her own anymore. A once vibrant, muscular, strong dog now depending on humans to get her outside, to get her on and off the couch. She was tired. And she was sad. Her eyes told me that she had had enough. She didn’t deserve to live with awful pain because “I” wanted her to be around longer. She deserved to be at peace, even though her peace meant pain, anger and grief for me.